Search
- Page Path
- HOME > Search
- Hypothalamus and pituitary gland
- Clinical Characteristics, Diagnosis, and Treatment of Thyroid Stimulating Hormone-Secreting Pituitary Neuroendocrine Tumor (TSH PitNET): A Single-Center Experience
- Jung Heo, Yeon-Lim Suh, Se Hoon Kim, Doo-Sik Kong, Do-Hyun Nam, Won-Jae Lee, Sung Tae Kim, Sang Duk Hong, Sujin Ryu, You-Bin Lee, Gyuri Kim, Sang-Man Jin, Jae Hyeon Kim, Kyu Yeon Hur
- Endocrinol Metab. 2024;39(2):387-396. Published online February 5, 2024
- DOI: https://doi.org/10.3803/EnM.2023.1877

- 1,412 View
- 38 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Thyroid-stimulating hormone (TSH)-secreting pituitary neuroendocrine tumor (TSH PitNET) is a rare subtype of PitNET. We investigated the comprehensive characteristics and outcomes of TSH PitNET cases from a single medical center. Also, we compared diagnostic methods to determine which showed superior sensitivity.
Methods
A total of 17 patients diagnosed with TSH PitNET after surgery between 2002 and 2022 in Samsung Medical Center was retrospectively reviewed. Data on comprehensive characteristics and treatment outcomes were collected. The sensitivities of diagnostic methods were compared.
Results
Seven were male (41%), and the median age at diagnosis was 42 years (range, 21 to 65); the median follow-up duration was 37.4 months. The most common (59%) initial presentation was hyperthyroidism-related symptoms. Hormonal co-secretion was present in four (23%) patients. Elevated serum alpha-subunit (α-SU) showed the greatest diagnostic sensitivity (91%), followed by blunted response at thyrotropin-releasing hormone (TRH) stimulation (80%) and elevated sex hormone binding globulin (63%). Fourteen (82%) patients had macroadenoma, and a specimen of one patient with heavy calcification was negative for TSH. Among 15 patients who were followed up for more than 6 months, 10 (67%) achieved hormonal and structural remission within 6 months postoperatively. A case of growth hormone (GH)/TSH/prolactin (PRL) co-secreting mixed gangliocytoma-pituitary adenoma (MGPA) was discovered.
Conclusion
The majority of the TSH PitNET cases was macroadenoma, and 23% showed hormone co-secretion. A rare case of GH/TSH/PRL co-secreting MGPA was discovered. Serum α-SU and TRH stimulation tests showed great diagnostic sensitivity. Careful consideration is needed in diagnosing TSH PitNET. Achieving remission requires complete tumor resection. In case of nonremission, radiotherapy or medical therapy can improve the long-term remission rate.

- Adrenal Gland
- Urinary Free Metanephrines for Diagnosis of Pheochromocytoma and Paraganglioma
- Jiyeon Ahn, Ji Yun Park, Gyuri Kim, Sang-Man Jin, Kyu Yeon Hur, Soo-Youn Lee, Jae Hyeon Kim
- Endocrinol Metab. 2021;36(3):697-701. Published online June 1, 2021
- DOI: https://doi.org/10.3803/EnM.2020.925

- 4,406 View
- 188 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Pheochromocytoma and paraganglioma (PPGL) is diagnosed through biochemical confirmation of excessive catecholamines in urine and plasma. Recent technological developments have allowed us to measure urinary free metanephrines; however, the diagnostic accuracy of these new methods and the diagnostic cutoff values have not been evaluated.
Methods
This is a retrospective study of 595 subjects, including 71 PPGL cases and 524 controls. PPGL was based on pathological confirmation. Subjects with no evidence of PPGL over 2 years were included in the control group.
Results
Urinary free metanephrines yielded similar area under the curve (AUC) to urinary fractionated metanephrines and plasma free metanephrines. However, urinary free normetanephrine yielded a better AUC than did urinary fractionated normetanephrine. The optimal cutoff for urinary free metanephrine and normetanephrine corrected for urinary creatinine yielded 97.2% sensitivity and 98.1% specificity.
Conclusion
Urinary free metanephrines are a reliable method for diagnosing PPGL in Asian populations compared with existing biochemical methods. -
Citations
Citations to this article as recorded by- Biochemical Assessment of Pheochromocytoma and Paraganglioma
Graeme Eisenhofer, Christina Pamporaki, Jacques W M Lenders
Endocrine Reviews.2023; 44(5): 862. CrossRef - Adrenal bleeding due to pheochromocytoma - A call for algorithm
Ewelina Rzepka, Joanna Kokoszka, Anna Grochowska, Magdalena Ulatowska-Białas, Martyna Lech, Marta Opalińska, Elwira Przybylik-Mazurek, Aleksandra Gilis-Januszewska, Alicja Hubalewska-Dydejczyk
Frontiers in Endocrinology.2022;[Epub] CrossRef
- Biochemical Assessment of Pheochromocytoma and Paraganglioma

- Clinical Study
- Association of Body Mass Index with the Risk of Incident Type 2 Diabetes, Cardiovascular Disease, and All-Cause Mortality: A Community-Based Prospective Study
- Ji Cheol Bae, Nam H. Cho, Jae Hyeon Kim, Kyu Yeon Hur, Sang-Man Jin, Moon-Kyu Lee
- Endocrinol Metab. 2020;35(2):416-424. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.416
- 8,123 View
- 156 Download
- 13 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Type 2 diabetes and cardiovascular disease (CVD) are the most important sequelae of obesity and the leading cause of death. We evaluated the association between body mass index (BMI) and the risk of incident type 2 diabetes, CVD, and all-cause mortality in a prospective study of a Korean population.
Methods
The shapes of the associations were modeled by restricted cubic splines regression analysis. After categorizing all subjects (n=8,900) into octiles based on their BMI levels, we estimated the hazard ratio (HR) for the association of categorized BMI levels with the risk of incident CVD and type 2 diabetes using a Cox’s proportional hazard analysis.
Results
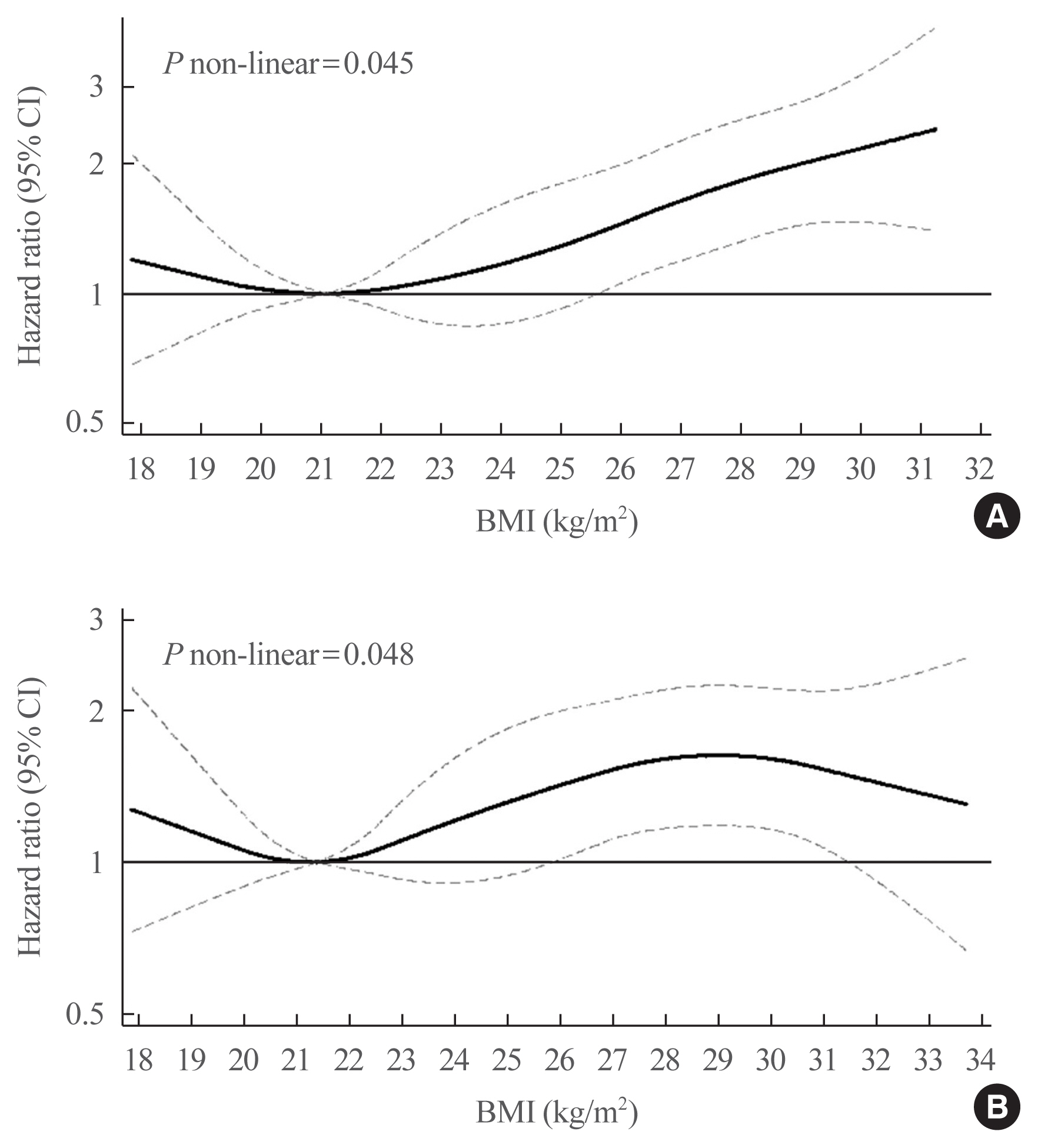
The mean age of participants was 52 years and 48% were men. Of the subjects at baseline, 39.0% of men and 45.6% of women were classified as obese (BMI ≥25 kg/m2). Over a mean follow-up of 8.1 years, CVD events occurred in 509 participants; 436 died; and 1,258 subjects developed type 2 diabetes. The increased risk of incident diabetes began to be significant at BMI 23 to 24 kg/m2 in both sexes (HR, 1.8). For CVD events, the risk began to increase significantly at BMI 26 to 28 kg/m2 (HR, 1.6). We found a reverse J-shaped relationship between BMI and all-cause mortality, with an increased risk among individuals with BMI values in lower range (BMI <21 kg/m2).
Conclusion
These results suggest that the BMI cut-off points for observed risk were varied depending on the diseases and that the BMI classification of obesity need to be revised to reflect differential risk of obesity-related diseases. -
Citations
Citations to this article as recorded by- Association of obesity with cardiovascular disease in the absence of traditional risk factors
Hui Luo, Yesong Liu, Xue Tian, Yuhan Zhao, Lulu Liu, Zemeng Zhao, Lili Luo, Yanmin Zhang, Xiaozhong Jiang, Yeqiang Liu, Yanxia Luo, Anxin Wang
International Journal of Obesity.2024; 48(2): 263. CrossRef - Clinical characteristics and degree of cardiovascular risk factor control in patients with newly-diagnosed type 2 diabetes in Catalonia
Anna Ramírez-Morros, Josep Franch-Nadal, Jordi Real, Queralt Miró-Catalina, Magdalena Bundó, Bogdan Vlacho, Didac Mauricio
Frontiers in Endocrinology.2024;[Epub] CrossRef - Metabolic status indicators and influencing factors in non-obese, non-centrally obese nonalcoholic fatty liver disease
Zhipeng Huang, Donghong Wei, Xueping Yu, Zicheng Huang, Yijie Lin, Wenji Lin, Zhijun Su, Jianjia Jiang
Medicine.2023; 102(6): e32922. CrossRef - Establishment and health management application of a prediction model for high-risk complication combination of type 2 diabetes mellitus based on data mining
Xin Luo, Jijia Sun, Hong Pan, Dian Zhou, Ping Huang, Jingjing Tang, Rong Shi, Hong Ye, Ying Zhao, An Zhang, Yee Gary Ang
PLOS ONE.2023; 18(8): e0289749. CrossRef - Differential Impact of Obesity on the Risk of Diabetes Development in Two Age Groups: Analysis from the National Health Screening Program
Tae Kyung Yoo, Kyung-Do Han, Yang-Hyun Kim, Ga Eun Nam, Sang Hyun Park, Eun-Jung Rhee, Won-Young Lee
Diabetes & Metabolism Journal.2023; 47(6): 846. CrossRef - Relationship between advanced lung cancer inflammation index and long-term all-cause, cardiovascular, and cancer mortality among type 2 diabetes mellitus patients: NHANES, 1999–2018
Yaying Chen, Mengqian Guan, Ruiqi Wang, Xuewen Wang
Frontiers in Endocrinology.2023;[Epub] CrossRef - Body mass index at baseline directly predicts new-onset diabetes and to a lesser extent incident cardio-cerebrovascular events, but has a J-shaped relationship to all-cause mortality
Yoon-Jong Bae, Sang-Jun Shin, Hee-Taik Kang
BMC Endocrine Disorders.2022;[Epub] CrossRef - Association of Shift Work with Normal-Weight Obesity in Community-Dwelling Adults
Chul Woo Ahn, Sungjae Shin, Seunghyun Lee, Hye-Sun Park, Namki Hong, Yumie Rhee
Endocrinology and Metabolism.2022; 37(5): 781. CrossRef - The Prognostic Value of Combined Status of Body Mass Index and Psychological Well-Being for the Estimation of All-Cause and CVD Mortality Risk: Results from a Long-Term Cohort Study in Lithuania
Dalia Lukšienė, Abdonas Tamosiunas, Ricardas Radisauskas, Martin Bobak
Medicina.2022; 58(11): 1591. CrossRef - The Relationship between Body Mass Index and Incident Diabetes Mellitus in Chinese Aged Population: A Cohort Study
M. L. Tang, Y. Q. Zhou, A. Q. Song, J. L. Wang, Y. P. Wan, R. Y. Xu, Carol Forsblom
Journal of Diabetes Research.2021; 2021: 1. CrossRef - Correlation between adiponectin level and the degree of fibrosis in patients with non-alcoholic fatty liver disease
Manal Sabry Mohamed, Tarek Mohammed Youssef, Esraa Ebrahim Abdullah, Ahmed Elmetwally Ahmed
Egyptian Liver Journal.2021;[Epub] CrossRef - Obesity Measures as Predictors of Type 2 Diabetes and Cardiovascular Diseases among the Jordanian Population: A Cross-Sectional Study
Hana Alkhalidy, Aliaa Orabi, Khadeejah Alnaser, Islam Al-Shami, Tamara Alzboun, Mohammad D. Obeidat, Dongmin Liu
International Journal of Environmental Research and Public Health.2021; 18(22): 12187. CrossRef
- Association of obesity with cardiovascular disease in the absence of traditional risk factors

- Stepwise Approach to Problematic Hypoglycemia in Korea: Educational, Technological, and Transplant Interventions
- Sang-Man Jin
- Endocrinol Metab. 2017;32(2):190-194. Published online June 23, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.2.190
- 3,127 View
- 34 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Impaired awareness of hypoglycemia has been found to be prevalent in 20% to 40% of people with type 1 diabetes. If a similar prevalence exists in Koreans with type 1 diabetes, at a minimum, thousands of people with type 1 diabetes suffer at least one unpredicted episode of severe hypoglycemia per year in Korea. For patients with problematic hypoglycemia, an evidence-based stepwise approach was suggested in 2015. The first step is structured education regarding multiple daily injections of an insulin analog, and the second step is adding a technological intervention, such as continuous subcutaneous insulin infusion or real-time continuous glucose monitoring. The next step is a sensor-augmented pump, preferably with a low glucose suspension feature or very frequent contact, and the final step is islet or pancreas transplantation. In Korea, however, none of these treatments are reimbursed by the National Health Insurance, and thus have not been widely implemented. The low prevalence of type 1 diabetes means that Korean physicians are relatively unfamiliar with the new technologies in this field. Therefore, the roles of new technologies and pancreas or islet transplantation in the treatment of problematic hypoglycemia need to be defined in the current clinical setting of Korea.
-
Citations
Citations to this article as recorded by- Protective and risk factors of impaired awareness of hypoglycemia in patients with type 1 diabetes: a cross-sectional analysis of baseline data from the PR-IAH study
Naoki Sakane, Ken Kato, Sonyun Hata, Erika Nishimura, Rika Araki, Kunichi kouyama, Masako Hatao, Yuka Matoba, Yuichi Matsushita, Masayuki Domichi, Akiko Suganuma, Seiko Sakane, Takashi Murata, Fei Ling Wu
Diabetology & Metabolic Syndrome.2023;[Epub] CrossRef - A 4-Week, Two-Center, Open-Label, Single-Arm Study to Evaluate the Safety and Efficacy of EOPatch in Well-Controlled Type 1 Diabetes Mellitus
Jiyun Park, Nammi Park, Sangjin Han, You-Bin Lee, Gyuri Kim, Sang-Man Jin, Woo Je Lee, Jae Hyeon Kim
Diabetes & Metabolism Journal.2022; 46(6): 941. CrossRef - Impaired hypoglycemia awareness in diabetes: epidemiology, mechanisms and therapeutic approaches
Vadim V. Klimontov
Diabetes mellitus.2019; 21(6): 513. CrossRef
- Protective and risk factors of impaired awareness of hypoglycemia in patients with type 1 diabetes: a cross-sectional analysis of baseline data from the PR-IAH study

- Adrenal gland
- Clinical Characteristics, Management, and Outcome of 22 Cases of Primary Hypophysitis
- Sun Mi Park, Ji Cheol Bae, Ji Young Joung, Yoon Young Cho, Tae Hun Kim, Sang-Man Jin, Sunghwan Suh, Kyu Yeon Hur, Kwang-Won Kim
- Endocrinol Metab. 2014;29(4):470-478. Published online December 29, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.4.470
- 4,249 View
- 41 Download
- 26 Web of Science
- 24 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Primary hypophysitis causes varying degrees of endocrine dysfunction and mass effect. The natural course and best treatment have not been well established.
Methods Medical records of 22 patients who had been diagnosed with primary hypophysitis between January 2001 and March 2013 were retrospectively reviewed. Based on the anatomical location, we classified the cases as adenohypophysitis (AH), infundibuloneurohypophysitis (INH), and panhypophysitis (PH). Clinical presentation, endocrine function, pathologic findings, magnetic resonance imaging findings, and treatment courses were reviewed.
Results Among 22 patients with primary hypophysitis, 81.8% (18/22) had involvement of the posterior pituitary lobe. Two patients of the AH (2/3, 66.6%) and three patients of the PH (3/10, 30%) groups initially underwent surgical mass reduction. Five patients, including three of the PH (3/10, 33.3%) group and one from each of the AH (1/3, 33.3%) and INH (1/9, 11.1%) groups, initially received high-dose glucocorticoid treatment. Nearly all of the patients treated with surgery or high-dose steroid treatment (9/11, 82%) required continuous hormone replacement during the follow-up period. Twelve patients received no treatment for mass reduction due to the absence of acute symptoms and signs related to a compressive mass effect. Most of them (11/12, 92%) did not show disease progression, and three patients recovered partially from hormone deficiency.
Conclusion Deficits of the posterior pituitary were the most common features in our cases of primary hypophysitis. Pituitary endocrine defects responded less favorably to glucocorticoid treatment and surgery. In the absence of symptoms related to mass effect and with the mild defect of endocrine function, it may not require treatment to reduce mass except hormone replacement.
-
Citations
Citations to this article as recorded by- Secondary xanthogranulomatous hypophysitis mimicking a pituitary macroadenoma: a case report
Salma Salhi, Ibtissem Oueslati, Yasmine Mouelhi, Alia Zehani, Nidhameddine Kchir, Elyes Kamoun, Meriem Yazidi, Melika Chihaoui
Journal of International Medical Research.2024;[Epub] CrossRef - Glucocorticoid therapy as first-line treatment in primary hypophysitis: a systematic review and individual patient data meta-analysis
Brijesh Krishnappa, Ravikumar Shah, Saba Samad Memon, Chakra Diwaker, Anurag R Lila, Virendra A Patil, Nalini S Shah, Tushar R Bandgar
Endocrine Connections.2023;[Epub] CrossRef - Hypophysitis, the Growing Spectrum of a Rare Pituitary Disease
Fabienne Langlois, Elena V Varlamov, Maria Fleseriu
The Journal of Clinical Endocrinology & Metabolism.2022; 107(1): 10. CrossRef - Outcomes of Initial Management Strategies in Patients With Autoimmune Lymphocytic Hypophysitis: A Systematic Review and Meta-analysis
Diane Donegan, Zeb Saeed, Danae A Delivanis, Mohammad Hassan Murad, Juergen Honegger, Felix Amereller, Seda Hanife Oguz, Dana Erickson, Irina Bancos
The Journal of Clinical Endocrinology & Metabolism.2022; 107(4): 1170. CrossRef - Early Pulse Glucocorticoid Therapy and Improved Hormonal Outcomes in Primary Hypophysitis
Brijesh Krishnappa, Ravikumar Shah, Vijaya Sarathi, Anurag Ranjan Lila, Manjeet Kaur Sehemby, Virendra A. Patil, Shilpa Sankhe, Nalini Shah, Tushar Bandgar
Neuroendocrinology.2022; 112(2): 186. CrossRef - Preoperative differentiation of hypophysitis and pituitary adenomas using a novel clinicoradiologic scoring system
Kyla Wright, Hyon Kim, Travis Hill, Matthew Lee, Cordelia Orillac, Nikita Mogar, Donato Pacione, Nidhi Agrawal
Pituitary.2022; 25(4): 602. CrossRef - Hypophysitis
Diane Donegan, Jürgen Honegger
Endocrine Practice.2022; 28(9): 901. CrossRef - Rare Case of a Disappearing Pituitary Adenoma During the Coronavirus Disease 2019 (COVID-19) Pandemic
David P. Bray, C. Arturo Solares, Nelson M. Oyesiku
World Neurosurgery.2021; 146: 148. CrossRef - Diabetes insipidus secondary to sellar/parasellar lesions
Anna Angelousi, Chrysoula Mytareli, Paraskevi Xekouki, Eva Kassi, Konstantinos Barkas, Ashley Grossman, Gregory Kaltsas
Journal of Neuroendocrinology.2021;[Epub] CrossRef - Clinical presentation and management of hypophysitis: An observational study of case series
Marouan Karrou, Salma Benyakhlef, Achwak Alla, Najoua Messaoudi, Asmae Oulad Amar, Siham Rouf, Imane Kamaoui, Noureddine Oulali, Faycal Moufid, Naima Abda, Hanane Latrech
Surgical Neurology International.2021; 12: 304. CrossRef - Clinical aspects of autoimmune hypothalamitis, a variant of autoimmune hypophysitis: Experience from one center
Qian Wei, Guoqing Yang, Zhaohui Lue, Jingtao Dou, Li Zang, Yijun Li, Jin Du, Weijun Gu, Yiming Mu
Journal of International Medical Research.2020; 48(3): 030006051988783. CrossRef - Primary and Ipilimumab-induced Hypophysitis: A Single-center Case Series
Paul Atkins, Ehud Ur
Endocrine Research.2020; 45(4): 246. CrossRef - Hypophysitis (Including IgG4 and Immunotherapy)
Anna Angelousi, Krystallenia Alexandraki, Marina Tsoli, Gregory Kaltsas, Eva Kassi
Neuroendocrinology.2020; 110(9-10): 822. CrossRef - Hypophysitis in the era of immune checkpoint inhibitors and immunoglobulin G4-related disease
Leen Wehbeh, Sama Alreddawi, Roberto Salvatori
Expert Review of Endocrinology & Metabolism.2019; 14(3): 167. CrossRef - Immune check point inhibitors-induced hypophysitis: a retrospective analysis of the French Pharmacovigilance database
Julie Garon-Czmil, Nadine Petitpain, Franck Rouby, Marion Sassier, Samy Babai, Mélissa Yéléhé-Okouma, Georges Weryha, Marc Klein, Pierre Gillet
Scientific Reports.2019;[Epub] CrossRef - Clinical Features, Magnetic Resonance Imaging, and Treatment Experience of 20 Patients with Lymphocytic Hypophysitis in a Single Center
Qiang Zhu, Ke Qian, Guijun Jia, Gang Lv, Jisheng Wang, Liyong Zhong, Shuqing Yu
World Neurosurgery.2019; 127: e22. CrossRef - Idiopathic granulomatous hypophysitis presenting with galactorrhea, headache, and nausea in a woman: a case report and review of the literature
Guive Sharifi, Mohammad Reza Mohajeri-Tehrani, Behrouz Navabakhsh, Bagher Larijani, Touraj Valeh
Journal of Medical Case Reports.2019;[Epub] CrossRef - Paciente de 31 años con polidipsia
A.R. Benavides Aramburu, M. Seguí Díaz
Medicina de Familia. SEMERGEN.2018; 44(2): e77. CrossRef - Primary hypophysitis and other autoimmune disorders of the sellar and suprasellar regions
Sriram Gubbi, Fady Hannah-Shmouni, Constantine A. Stratakis, Christian A. Koch
Reviews in Endocrine and Metabolic Disorders.2018; 19(4): 335. CrossRef - Primary lymphocytic hypophysitis: Clinical characteristics and treatment of 50 cases in a single centre in China over 18 years
Shuchang Wang, Linjie Wang, Yong Yao, Feng Feng, Hongbo Yang, Zhiyong Liang, Kan Deng, Hui You, Jian Sun, Bing Xing, Zimeng Jin, Renzhi Wang, Hui Pan, Huijuan Zhu
Clinical Endocrinology.2017; 87(2): 177. CrossRef - Clinical presentation and outcome of children with central diabetes insipidus associated with a self‐limited or transient pituitary stalk thickening, diagnosed as infundibuloneurohypophysitis
J. Schaefers, M. Cools, K. De Waele, I. Gies, V. Beauloye, P. Lysy, I. Francois, D. Beckers, J. De Schepper
Clinical Endocrinology.2017; 87(2): 171. CrossRef - Intrachiasmatic abscess caused by IgG4-related hypophysitis
Georgios F. Hadjigeorgiou, Eva Løbner Lund, Lars Poulsgaard, Ulla Feldt-Rasmussen, Åse Krogh Rasmussen, Marianne Wegener, Kåre Fugleholm
Acta Neurochirurgica.2017; 159(11): 2229. CrossRef - Granulomatous and lymphocytic hypophysitis – are they immunologically distinct?
Shilpa Rao, Anita Mahadevan, Tanmoy Maiti, Manish Ranjan, Shivayogi Durgad Shwetha, Arimappamagan Arivazhagan, Jitender Saini
APMIS.2016; 124(12): 1072. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef
- Secondary xanthogranulomatous hypophysitis mimicking a pituitary macroadenoma: a case report


 KES
KES

 First
First Prev
Prev



